Kamagra gibt es auch als Kautabletten, die sich schneller auflösen als normale Pillen. Manche Patienten empfinden das als angenehmer. Wer sich informieren will, findet Hinweise unter kamagra kautabletten.
Doi:10.1016/j.prrv.2006.06.003
PAEDIATRIC RESPIRATORY REVIEWS (2006) 7, 185–190
MINI-SYMPOSIUM: TRACHEOSTOMY IN CHILDREN
Tracheostomy care in the home
Be´atrice Oberwaldnerand Ernst Eber
Respiratory and Allergic Disease Division, Paediatric Department, Medical University of Graz,Auenbruggerplatz 30, A-8036 Graz, Austria
Summary There are hardly any controlled studies in paediatric tracheostomy care;
instead, most established standards, procedures and details have been elaborated at the
domiciliary care;
bedside by trial and error. Once the appropriate tube is chosen, tube care consists of tube
endotracheal suctioning;
change, fixation, management of secretions, humidification of inspired air and application
of medications. The stoma requires cleaning, protection and dressing. Child care may be
teaching programme for
structured into monitoring, feeding, bathing and clothing. Preparing the home and family
environment are important prerequisites for discharge from the hospital. Last but not
least, the family of the child or other caregivers must undergo a structured and detailedtraining programme to become competent in long-term home care.
ß 2006 Elsevier Ltd. All rights reserved.
Most tracheostomies performed for the former indica-
tion can be removed once the underlying pathology has
Since tracheostomies in children are almost exclusively
been corrected surgically or has ameliorated with growth
used as a long-term artificial airway, long-term caregiving
and development of the airway; tracheostomies for venti-
concepts have had to be developed. Children with a
latory support can also be removed once ventilation can be
chronic tracheostomy face the potential hazards of airway
applied non-invasively. Long-term management differs
compromise, and optimal care aims at reducing this risk.
between these two groups in terms of decannulation
Most caregiving strategies, standards, procedures and
protocols and control investigations; however, tube selec-
details have been developed by trial and error at the
tion (discussed elsewhere), tube care, stoma care and the
bedside; even nowadays, recommendations for optimal
education and training of caregivers are essentially the
care stem rather from the consensus of experts rather
than from controlled
In many ways, long-term management depends on the
indication for tracheostomy. In a chronically obstructed
upper airway, tracheostomy is used for bypassing the
stenosis; in the presence of tracheomalacia, a tracheostomytube may also be used to stent the airway. Where there is a
The frequency of tube change depends on the material of
chronic need for invasive ventilatory support as well as for
the tube and the presence of infection and/or secretions.
management of secretions, tracheostomy is used for
The polyvinyl chloride material, most widely used for
directly accessing the airway.
paediatric tracheostomy tubes, allows the tubes to stayin place for several weeks, although inspissated secretionsoccasionally call for more frequent changes. If tubes are
* Corresponding author. Tel.: +43 316 385 84597;
reusable, it is essential to inspect the tube for possible
Fax: +43 316 385 3276.
damage and for reduced flexibility with time and repeated
(B. Oberwaldner).
1526-0542/$ – see front matter ß 2006 Elsevier Ltd. All rights reserved.
doi:
B. OBERWALDNER AND E. EBER
In the case of a very tight stoma, the tissue layers
between skin and trachea tend to close or narrow the
In children with a tracheostomy, airway patency is main-
stoma channel by shifting differently; therefore, changing
tained by suctioning of the tube.
the tube may be difficult. It can be accomplished bythreading the new tube over a guiding structure such asan appropriately sized suction tube. A smaller tube and
Frequency (timing) of suctioning
ambubag should be within easy reach in case of insertion
Suctioning is best performed on an as-needed basis, the
frequency depending on the child's ability to generate aneffective cough and on viscosity and amount of secretions.
Consequently, caregivers must be trained to assess com-petently the need for removal of secretions, and suction
Various materials, such as Velcro ties, twill tapes, elastic
equipment must be with the child at all times. Suctioning on
straps with hooks and stainless steel chains, are available to
a routine basis is restricted to children with hardly any
secure the tube in place. In children, especially in those with
secretions and should then be performed at least in the
tracheostomies for bypassing an obstructed upper airway,
morning and evening in order to ensure continued patency
preventing accidental decannulation is vital. Hence a twill
of the tube.
tape, securely tied with triple square knots to both sides ofthe neck flange, is the most reliable option. As these tapestend to shrink with moisture and might then cause skin
Depth of suctioning
irritation or even compromise of the venous return, thread-ing the tape through a silicone tube is recommended. This
Shallow suctioning. A pre-measured length of the catheter is
protects the skin and allows for easy cleaning underneath.
inserted to a depth where the side-holes reach the tip of
When a fresh tape is needed, a recommended procedure,
the tube. This technique avoids mucosal damage and
which is safe even in a young active baby, is to tie the new
irritation; however, it also carries some risk of encrusted
over the old one and cut the latter only once the tube has
secretions and consecutive tube obstruction in case the
been secured by the new tape. Velcro tapes are reserved
catheter does not fully reach the end of the tube. Exact
for children in whom accidental decannulation would not
measurement of tube length and catheter insertion depth
cause serious adverse events. Elastic straps with hooks as
are prerequisites for correct suction technique.
well as chains should not be used in children.
Deep suctioning. This means inserting the catheter until
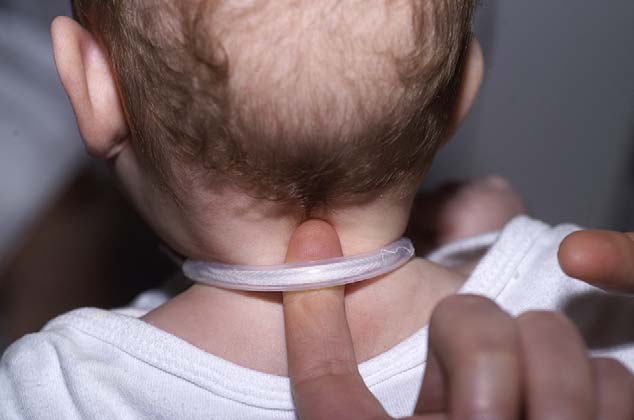
Tapes should be tight enough to prevent accidental
resistance is met and applying suction only on withdrawal.
decannulation yet loose enough to allow for a change in
Because of the risk of epithelial damage, this technique
neck size during laughing, crying and feeding. The correct
should never be used as a routine; however, in selected
tension is given when one finger can be slipped without
situations, it can be necessary for clearance of secretions
force beneath the tape at the back of the flexed neck
located beyond the tube.
All adjuncts fitted onto the tracheostomy tube, such as
Suction equipment
breathing circuits, heat and moisture exchangers, as well asspeaking valves, should be secured in a way that avoids
Suction pump. Depending on his or her mobility, the child
tension on the tube ).
has to be equipped with two or three different suctionpumps. A stationary suction pump must have a manometerfor setting the suction pressure and should be capable ofgenerating the preset vacuum rapidly. It should be equippedwith an easily removable bottle that is big enough forholding a day's suction volume.
An additional portable suction pump must be able to
run on batteries for a considerable time span, should belight-weight and ought to be equipped with a valvemechanism to prevent spill-over of secretions into themotor during transportation. Finally, a hand or foot pumpis necessary to allow for suctioning independent ofelectricity.
Suction catheters. Catheters, marked longitudinally for
easy control of insertion depth, are preferred. They musthave an ideal combination of flexibility and stability to
Tube fixation. Checking for the correct tension of the
facilitate a quick and easy pass. A rounded end-hole and
several side-holes close to the end of the catheter clear
TRACHEOSTOMY CARE IN THE HOME
Saline instillation
When no secretions are present in the tube, a sterile 0.9%sodium chloride solution can be instilled in order to elicit acough, which transports secretions from the peripheralairways towards the tube. When secretions are presentin the tube, there is no need for saline instillation. In fact,saline instillation could then have the negative effect ofwashing secretions down into the lung periphery, therebyincreasing resistance and decreasing oxygen saturation. Ifsaline is used, it should never be bagged down the tubebecause of the risk of carrying infectious material into theperipheral airways.
Bag ventilation/reinstitution of functional residualcapacity after suctioning
In spontaneously breathing children who need lengthysuctioning, restoration of lung volume is essential to preventatelectasis and reduce dyspnoea after suctioning. An ade-quately sized bag, equipped with a positive end-expiratorypressure (PEEP) valve (with an individually set PEEP level), isconnected to the tracheostomy tube, and, in coordinationwith the child's respiration, several slow inspirations areapplied.
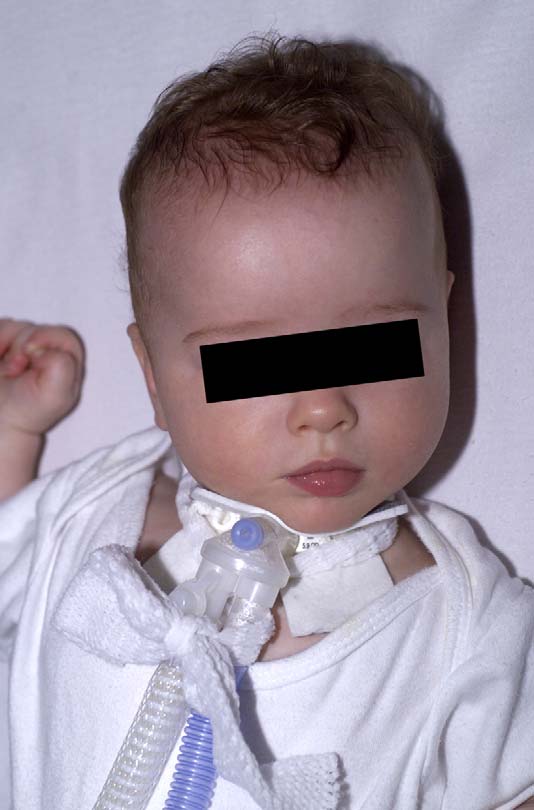
Set-up for mechanical ventilation. Observe the extra
Suction procedure
fixation of the tubing and the padding of the chin by the stomadressing.
Tube length and depth of insertion to the tip of the tube arenoted before suctioning. When secretions are present inthe tube (suctioning on demand), the catheter is inserted to
secretions from the tip and the inside of the tube. The top
the premeasured depth with already applied negative
end of the catheter should carry a hole that can be opened
pressure in order to prevent pushing secretions further
or occluded by the operator's thumb for interrupting or
down the airway. Using a catheter with an outer diameter
recommencing suction as needed.
of approximately 75% of the tube's lumen provides for arapid removal of secretions. For routine suction, a smaller
catheter (outer diameter approximately 50% of the lumen)is inserted without negative pressure in order to prevent
Depending on the length and internal diameter of the
loss of lung volume during a more lengthy search for
catheter, the suction pressure at the end of the catheter
is variable. Suction pressures should be set between 80 and
On withdrawal, the catheter is twisted between the
150 mm Hg; gauging the pressures is essential.
fingers for clearing secretions from as much of the innerwall of the tube as possible. After the tube has been cleared
Clean versus sterile technique
of secretions, bag ventilation is used to restore lung volume.
In the home, a clean technique (freshly washed hands and a
sterile, non-reusable catheter) will most likely suffice. In thehospital, as well as out of the home, when hand-washing is
Since the upper airway is bypassed by the tracheostomy,
not possible, a sterile technique (sterile glove and catheter)
the inspired air will be neither sufficiently warmed nor
should be used.
humidified, thereby compromising ciliary action and inspis-sating secretions. Occasionally, it might therefore be neces-sary to actively humidify the tracheostomy. For this
Duration of suction
purpose, pressurised air is directed through a heated water
A rapid technique reduces the risk of development of
bath into tubing connected to a tracheostomy collar. Ideally,
atelectasis. With adequate suction pressure and a firm
inspired air should contain approximately 36–40 mg of
catheter with longitudinal marks, effective suctioning can
water per litre of air at 32 8C. Such conditions can only
be performed in a few seconds.
be achieved with cumbersome technical equipment; con-
B. OBERWALDNER AND E. EBER
sequently, such a maximally effective humidification is only
can be removed with a cotton wool swab and normal
practicable in a sedentary child or during sleep. Otherwise,
saline. Around the stoma, the skin should be kept dry and
the tracheostomy should be equipped with a passive
liquid creams avoided. In case of fungal infections or
humidifier (‘artificial nose') that traps exhaled vapour and
inflammation, adequate ointments can be used cautiously
temperature and redelivers some of this during inspiration.
for a short period of time.
Weight, resistance, dead space and hygroscopic capacity
are important characteristics of these humidifiers. For
children, wearing a speaking valve for longer periods ofthe day, humidifiers will not work because exhalation does
A partially slit dressing, with a key hole for accommodating
not use the same route as inhalation. If dryness of secretions
the tube and made of non-fluffy and water-permeable
is evident, a speaking valve equipped with a filter inside the
material, helps to keep the skin around the stoma dry. In
valve can ameliorate the problem.
case of a short distance between the chin of a baby and thecannula, these dressings also serve as padding when used
Application of drugs
with the closed side under the chin In case ofdischarge from the stoma, the dressing can provide some
Various drugs can be administered via a tracheostomy for a
protection for clothes when it is slipped under the neck
local or systemic therapeutic effect.
plate from below.
Sometimes granulation tissue around the stoma inter-
feres with the snug fit of the tube; this problem can betackled with silver nitrate dressings or silver nitrate sticks.
Bronchodilators and anti-inflammatory drugs can be admi-nistered effectively by a metered-dose inhaler (MDI)equipped with a valved holding chamber. A special holding
chamber with a non-rebreathing valve and a connector to
fit onto the tube can be used in children with inspiratoryflows that are sufficient for opening the valve and emptying
When the continuous presence of a competent caregiver is
the chamber. In children who are unable to generate these
not available, the child should always be connected to a
flows, an ambubag connected to the holding chamber can
monitoring device. Ideally, a monitor should provide for an
facilitate drug delivery. An MDI plus holding chamber is
early and reliable warning of airway compromise. Alarms
better than a nebuliser for aerosol deposition distal to the
need to be set individually, and caregivers should be trained
tracheostomy tube.
to stay alert despite the occurrence of unavoidable falsealarms.
Antibiotics that are not available as a per os formula can be
instilled for local infection control. Diluting the drug to an
Even if swallowing is no problem and a baby is capable of
optimal osmolality, warming it, and instilling it slowly drop
holding a bottle, he or she should only do so under
by drop prevents irritation and helps to avoid coughing or
supervision, because accidental disconnection of the
demand for suctioning. Bagging the droplets carefully down
sucker may result in massive aspiration via the tracheost-
towards the lower airways can be useful in tubes with a
In children who are tube-fed for a certain length of time,
By the drug's direct action in the lung, the effective dose
oral food intake may cause some problems. In these, as well
might be lower than the comparable i.v. dose.
as in children with additional neurological disorders, speechtherapists should be consulted.
Emergency intravenous drugs
In emergency situations, where no intravenous access is
readily available, drugs such as atropine, epinephrine and
A bath with a water level not higher than the child's
lidocaine show a systemic effect when administered endo-
abdomen is safe for the young patient who is under
constant supervision. Care must be taken to preventaspiration of splash water. Bath toys such as buckets and
STOMA (SKIN) CARE
water pistols should not be allowed. When washing hair, awaterproof protector (like a collar) should be used if the
child cannot extend or flex the head far enough to direct
The skin around the neck is cleaned with a wet but not
the water away from the stoma. Showering that carefully
dripping cloth. Encrusted secretions under the neck plate
avoids the head and neck is safe for older children.
TRACHEOSTOMY CARE IN THE HOME
cause substantial stress. Increased attention to the childand insecurity concerning disciplinary measures can cause
Clothing should not consist of furry or fluffy materials. To
jealousy and resentment in the rest of the family; social
prevent accidental decannulation, dressing and undressing
isolation as well as physical and emotional overload may
must not be over the head. High necks could occlude or
follow. To prevent burnout, additional caregivers have to
dislodge the tube and should therefore be avoided.
be recruited and trained, and community resources utilised.
It often helps caregivers to consult with support groups and
Preparing the home environment
establish links with other families who have successfully
The home into which a child with a tracheostomy is to be
cared for a child with a tracheostomy. Provision needs to be
discharged often needs adaptations that have to be planned
made well in advance for accommodating the child in
with the help of the health-care team well in advance.
playgroup, kindergarten and school.
When, due to the underlying pathology, voice genera-
tion fails, other ways of communication, such as an elec-
trolarynx, sign language or a letter board, need to be
Additional electricity sockets around the bed and in the
considered in order prevent isolation of child and family.
child's living area, as well as some extra space for storingdisposable utensils, are needed. Bath/shower facilities mustbe adapted to provide safety and to suit both child and
caregivers. Occasionally, a clever rearrangement of rooms
will substantially facilitate caregiving and monitoring. In caseof room-sharing between siblings, one must consider the
A structured training protocol, tailored to the needs of the
disturbance of the co-sleeper by alarms and various care
individual child and equipment, has proved to be useful. The
measures. Transporting the child together with all neces-
achievements of the trainee caregivers are monitored step
sary equipment often calls for adaptation of staircases, car
by step in an appropriate log book.
seats, prams, etc.
Education is started preferably before elective tracheot-
omy; topics include indications for tracheostomy, the rele-vant anatomy and physiology, and differences form ‘normal'
breathing. Models, drawings and videos provide support for
Hazards for the child with a tracheostomy need to be
understanding the often complex situation. During the
identified and removed wherever possible. Exposure to
postoperative period, parents are encouraged to spend
feathery or furry pets, garden sprinklers, fountains, swim-
as much time as possible with their child in order to gain
ming pools, sand pits and powdery building or cleaning
confidence in mastering the expected challenge of having a
material, as well as air pollution by pollen, smoke, mist and
child with a tracheostomy at home.
household sprays, must be avoided.
Feeding, bathing, lifting the child out of bed, cuddling and
carrying are demonstrated and gradually taken over by theparents. Once they feel confident with handling their child,
teaching progresses to stoma and tube care as well as to
Well before discharge, communication with the family
monitoring vital signs. Special emphasis is directed towards
doctor, paediatrician, pharmacist, nurse specialist, when
a correct suction technique, and mock emergency situa-
applicable also speech pathologist and physiotherapist as
tions as well as the appropriate resuscitation measures are
well as equipment supplier should be established. A tele-
discussed and practised over and over again. The equip-
phone connection and power supply must be secured.
ment purchased for domiciliary care should already be usedon the ward to practice correct handling, cleaning, main-tenance and trouble-shooting.
Once all necessary knowledge and skills have been
Home tracheostomy care is a considerable burden and
obtained and the child is ready to go home, the caregivers
challenge for any family; commitment to provide optimal
are admitted together with their child onto a side ward,
care in the home and a conviction that home care is the
where they can practise the home situation day and night
best for the child's social, communicative and motor devel-
and see for themselves whether they are competent and
opment helps caregivers to cope with this challenge and
confident enough. An emergency package should be with
strive for a family life as near to normal as possible. As a
the child at all times. This must contain a spare tube of same
prerequisite for tracheostomy home care, caregivers have
size and one size smaller, scissors, ties, suction catheters,
to acquire the necessary knowledge and become compe-
normal saline, gloves and an ambubag with appropriate
tent in a spectrum of practical skills.
mask, together with an information card to quickly identify
Once the child is in the home, parental responsibility is
brand, size and length of tube, catheter insertion depth, the
massive; anxiety and preparedness for an emergency may
reason for the tracheostomy, potential individual risks and

B. OBERWALDNER AND E. EBER
the names and telephone numbers of physicians, therapists,
2. Carr MM, Poje CP, Kingston L, Kielma D, Heard C. Complications in
nurses and service and maintenance companies.
pediatric tracheostomies. Laryngoscope 2001; 111: 1925–1928.
3. Alladi A, Rao S, Das K, Charles AR, D'Cruz AJ. Pediatric tracheostomy:
a 13-year experience. Pediatr Surg Int 2004; 20: 695–698.
4. American Thoracic Society. Care of the child with a chronic tra-
cheostomy. Am J Respir Crit Care Med 2000; 161: 297–308.
In summary, caring for a child with a chronic tracheostomy
5. Oberwaldner B. Tracheostoma. In: Rieger C, von der Hardt H,
Sennhauser FH, Wahn U, Zach M, eds: Pa¨diatrische Pneumologie.
in the home provides a challenge that can be met con-
Berlin: Springer, 2004; pp. 412–417.
fidently by a package of optimal medical management,
6. Fiske E. Effective strategies to prepare infants and families for home
motivated caregivers, adequate training and education, a
tracheotomy care. Adv Neonatal Care 2004; 4: 42–53.
well prepared and equipped home environment, support
7. Oberwaldner B, Zobel G, Zach M. Pa¨diatrische Tracheostomapflege.
from the extended family and community, and well-estab-
Monatsschr Kinderheilkd 1992; 140: 206–215.
8. Oberwaldner B. Physiotherapie. In: Rieger C, von der Hardt H,
lished communication with the health-care team. With
Sennhauser FH, Wahn U, Zach M, eds: Pa¨diatrische Pneumologie.
these prerequisites, domiciliary tracheostomy care is as
Berlin: Springer, 2004; pp. 379–389.
safe as, and in many other aspects superior to, long-term
9. Bailey C, Kattwinkel J, Teja K, Buckley C. Shallow versus deep
endotracheal suctioning in young rabbits: pathologic effects on thetracheobronchial wall. Pediatrics 1988; 82: 746–751.
10. Kerem E, Yatsiv I, Goitein KJ. Effects of endotracheal suctioning on
arterial blood gases in children. Intensive Care Med 1990; 7: 227–231.
11. Raymond S. Normal saline instillation before suctioning: helpful or
harmful? A review of the literature Am J Crit Care 1995; 4: 267–271.
The authors would like to thank Professor M. Zach, Graz,
12. Schwenker D, Ferrin M, Gift AG. A survey of endotracheal suctioning
with instillation of normal saline. Am J Crit Care 1998; 7: 255–260.
Austria, for reviewing this manuscript and for his valuable
13. Dajlby RW, Hogg JC. Effect of breathing dry air on structure and
function of airways. J Appl Physiol 1980; 61: 312–317.
14. Branson RD, Davis K Jr. Evaluation of 21 passive humidifiers according
to the ISO 9360 standard: moisture output, dead space and flowresistance. Respir Care 1996; 41: 736–743.
15. Lewarski JS. Long-term care of the patient with a tracheostomy. Respir
Care 2005; 50: 534–537.
� Tracheostomy care can be safely performed in the
16. Piccuito CM, Hess DR. Albuterol delivery via a tracheostomy tube.
Respir Care 2005; 50: 1071–1076.
� It is essential that all caregivers are appropriately
17. Mirza S, Hopkinson L, Malik TH, Willatt DJ. The use of inhalers in
patients with tracheal stomas or tracheostomy tubes. J Laryngol Otol
trained in all aspects of tracheostomy care and the
1999; 113: 762–764.
management of relevant emergency situations.
18. Fitton C, Myer CM III. Home care of the child with a tracheostomy. In:
� All necessary equipment for routine and emer-
Myer CM, III, Cotton RT, Shott SR, eds: The Pediatric Airway–an
gency care, together with a competent caregiver,
Interdisciplinary Approach. Philadelphia: JB Lippincott, 1995; pp. 171–
must be with the child at all times.
19. Bryant K, Davis C, Lagrone C. Streamline discharge planning for
� The home environment should be adequately
the child with a new tracheotomy. J Pediatr Nurs 1997; 12: 191–192.
adapted and equipped ahead of time once the
20. Buzz-Kelly L, Gordin P. Teaching CPR to parents of children with
decision to carry out future domiciliary care is
tracheostomies. MCN Am J Matern Child Nurs 1993; 18: 158–163.
21. Carnevale FA, Alexander E, Davis M, Rennick J, Troini R. Daily
� Family burnout can be prevented by the recruit-
living with distress and enrichment: the moral experience offamilies with ventilator assisted children at home. Pediatrics 2006;
ment and training of additional caregivers and the
117: 48–60.
utilisation of community resources.
22. Messineo A, Giusti F, Narne S, Mognato G, Antoniello L, Guglielmi M.
The safety of home tracheostomy care for children. J Pediatr Surg 1995;30: 1246–1248.
23. Fitton C. Nursing management of a child with a tracheostomy. Pediatr
Clin North Am 1994; 3: 513–523.
1. Shinkwin CA, Gibbin KP. Tracheostomy in children. J R Soc Med 1996;
24. Barnes LP. Tracheostomy care: preparing parents for discharge. MCN
89: 188–192.
Am J Matern Child Nurs 1992; 17: 293.
Source: http://www.canule.nl/doc/careinhome.pdf
Received 11.18.05 Revisions Received 1.26.06 Accepted 2.2.06 Validating New Reagents: Roadmaps Through the WildernessRoberta A. Martindale, BSc (MLS), MT(ASCP),1 George S. Cembrowski MD, PhD,1,2 Lucille J. Journault,1,2 Jennifer L. Crawford,BSc (MLS),1,2 Chi Tran,1,2 Tammy L. Hofer, BSc (MLS), MBA,1,2 Bev J. Rintoul, BSc (MLS)1,2 Jean S. Der,1,2 Cathy W. Revers, BSc (MLS),1,2 Cheryl A. Vesso,1,2 Carol E. Shalapay,1,2 Connie I. Prosser, PhD, FCACB,1,2 Donald F. LeGatt, PhD, FCACB1,2( 1Department of Laboratory Medicine and Pathology, University of Alberta Hospitals, 2Capital Health Authority, Edmonton, Canada)
Contents lists available at Complementary Therapies in Clinical Practice Pilates for low back pain: A systematic review Paul Posadzki ,, Pawel Lizis , Magdalena Hagner-Derengowska a Complementary Medicine, Peninsula Medical School, 25 Victoria Park Road, Exeter, Devon EX2 4NT, UKb Institute of Physiotherapy, Saint Cross Physiotherapy College, Kielce, Polandc Rehabilitation Clinic, Department of Health Sciences, Collegium Medicum, Nicolas Copernicus University, Bydgoszcz, Poland



